INTRODUCTION
Obstructive jaundice in patients with hepatocellular carcinoma (HCC) unusually presents in 1-12% as the initial symptom at the time of diagnosis[1]. This may be caused by biliary involvement of HCC in several ways: tumor thrombi and hemorrhagic clot, external compression by direct tumor encasement or the metastatic lymphadenopathy in the porta hepatis, or direct tumor invasion[2,3]. Of these causes, authors had the opportunity to diagnose and treat a case of biliary invasion of HCC. A few cases reported successful surgical treatments of HCC invading into biliary tract[4-6]. However, they undergo non-surgical treatments such as endoscopic retrograde biliary drainage (ERBD) or percutaneous transhepatic biliary drainage (PTBD) to improve obstructive jaundice and allow further palliative therapy such as transcatheter arterial chemoembolization (TACE) and chemotherapy, because most patients are inoperable. These patients, in spite of palliative treatments, mostly have sustained biliary drainage devices to relieve jaundice and to prolong survival. However, a recent study reported that the median survival was longer in patients who underwent TACE after achieving successful drainage than in patients who were treated conservatively after achieving successful drainage[7]. In addition, our case presents a completely resolved biliary invasion of inoperable HCC after TACE as a palliative treatment.
CASE
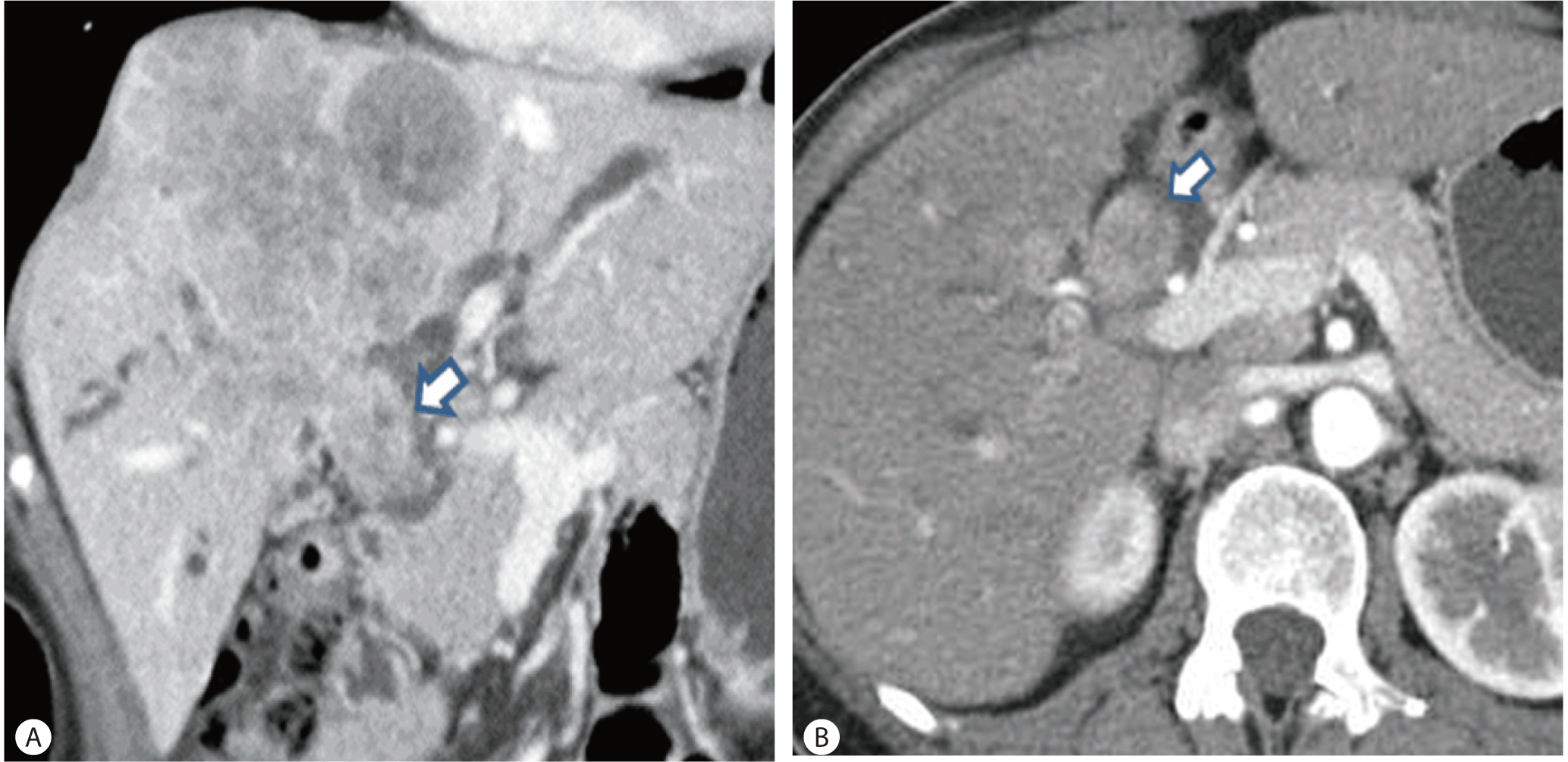
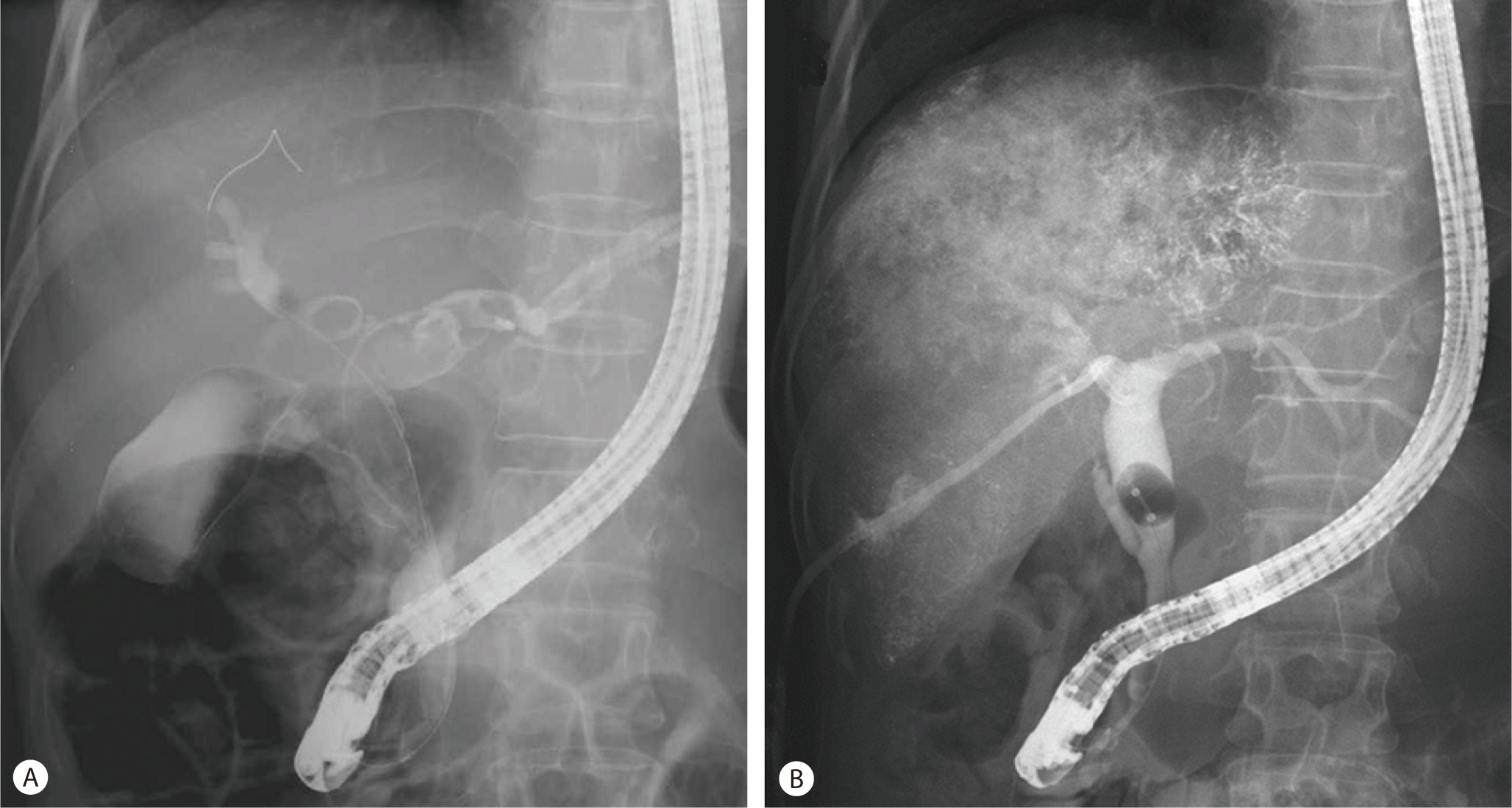
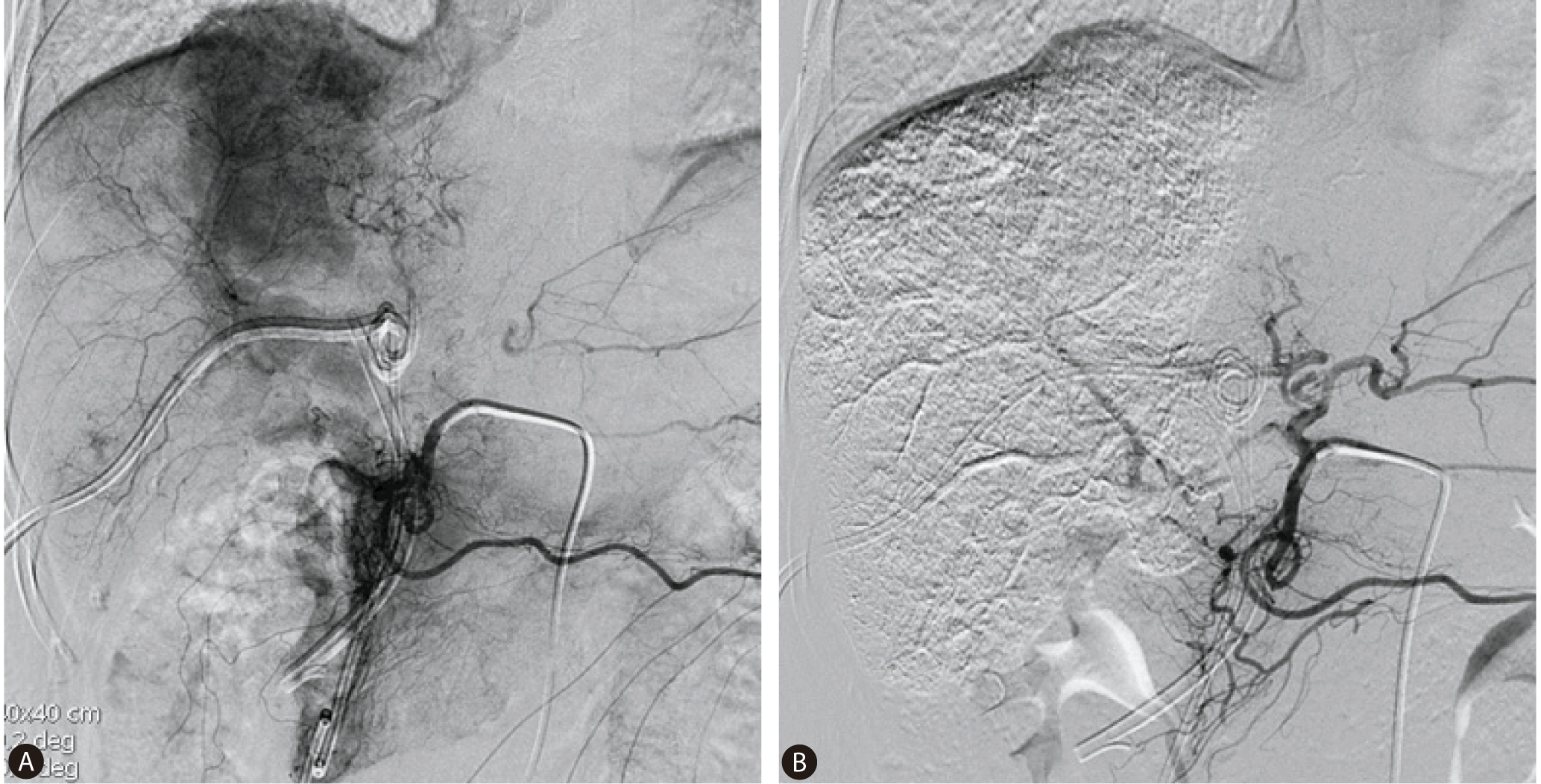
A 61-year-old woman was referred for evaluation of jaundice. She had neither previous history of chronic liver disease nor heavy alcohol-drinking. There was no hepatotoxic medication in her drug history. On the admission day, laboratory chemistry showed the serum total and direct bilirubin was 9.23 and 4.88 mg/dL, respectively. The serum alpha fetoprotein (AFP) was moderately elevated as 47 ng/ml (normal range, <8.1 ng/mL). Negative serology excluded viral hepatitis. Abdominal computerized tomography (CT) showed huge and multi-nodular tumors of both lobes, dilated intrahepatic bile ducts, and a direct tumor invasion in the common bile duct (Fig. 1A, 1B). And, endoscopic retrograde cholangiopancreatography (ERCP) showed an invasion accompanied with tumor emboli from the first branch of both intrahepatic bile duct to common bile duct (Fig. 2A). Endoscopic ultrasound examination was performed to characterize the nature of intraductal mass and the involvement to adjacent organ. It showed an intraductal hypo-echoic mass that was well demarcated with bile duct wall (Fig. 3A, 3B). The biliary invasion of HCC was confirmed by histologic findings of tissue specimen acquired from endoscopic ultrasound-guided fine needle aspiration (EUS-FNA) (Fig. 3C, 3D). The patient underwent endoscopic retrograde biliary drainage (ERBD) for obstructive jaundice. But, on the 4th admission day, she underwent percutaneous transhepatic biliary drainage (PTBD) due to insufficient bile drainage. One week later, the total and direct bilirubin was dramatically decreased below to 2.4 and 1.3 mg/dL, respectively. On the 13th admission day, TACE was done as a palliative treatment (Fig. 4A, 2B). Follow-up abdominal CT at 4 weeks later after TACE showed partial lipiodol uptake in the hepatic tumors and the tumor of bile duct invasion. The serum bilirubin was normalized after TACE. So we tried to remove drainage catheter and stent by PTBD and ERBD. After removal of the stent, she had sustained in normal range of the serum bilirubin and biliary occlusion had been resolved. And follow-up ERCP showed that there was neither luminal obstruction nor filling defect (Fig. 2B).
DISCUSSION
Jaundice in HCC is rarely caused by obstruction of the bile ducts by the tumor. This was attributed to one of the following mechanisms[2,3]: (1) a tumor may erode into a branch of biliary tree and grow distally until it occlude the entire extra-hepatic biliary tree to form a biliary tumor thrombus; (2) a necrotic free-floating fragment of tumor may separate from the biliary tumor and migrate distally to obstruct the common bile duct; (3) bleeding from the biliary tumor may occlude the biliary tree with blood clots; (4) the presence of malignant porta hepatis lymph nodes can compress the common hepatic or bile duct leading to extra- hepatic biliary obstruction; (5) direct tumor invasion or (6) external compression by direct tumor encasement give rise to localized strictures with proximal ductal dilatation. Considering abdominal CT and biopsy slides of EUS-FNA, our case revealed that direct invasion of HCC into biliary tract caused obstructive jaundice. After diagnosis, we evaluated the application of the Barcelona clinic liver cancer (BCLC) staging classification to access treatment[8]. Considering the huge and multi-nodular tumors, the Okuda stage II with the serum total bilirubin >3 mg/dL, the Child-Pugh classification B, and the performance status stage 1 with jaundice symptom, she was already in advance stage and was inoperable. But there was neither portal vein invasion nor metastasis. Bruix et al. recommended TACE as a first line non-curative therapy for non-surgical patients with large/multifocal HCC without vascular invasion or extra-hepatic spread[9]. So she underwent TACE as a palliative therapy. As a result, the biliary invasion of HCC was unexpectedly improved enough to resolve jaundice successfully. Theoretically, TACE achieves two goals: delivery of concentrated chemotherapeutic agent to the site of disease and interruption of hepatic arterial flow to the tumor[10]. The progression of HCC is mostly dependent on the hepatic artery for blood supply and tumor presents more intense neo-angiogenic activity[9]. This supports arterial embolization as the more effective therapeutic strategy in a lesion mainly receiving hepatic artery supply. Considering this rationale in our case, we supposed that blood supply of the biliary invasion became mostly arterialized with hepatic artery. So the invasive tumor was more dramatically necrotized by TACE.
The ideal goal of surgical treatments of HCC with biliary invasion is a curative hepatic resection including the primary tumor and biliary invasion. Only limited articles reported successful surgical treatments of HCC invading into biliary tract[4-6]. Tanoue et al.[4] emphasized curative operation of biliary invasion by HCC is expected, when the tumor does not occupy the opposite lobe and there is no tumor cell in the bile obtained though percutaneous transhepatic cholangiography. However, most of these patients are not eligible for operation. Wang et al.[11] reported that there was no difference in survival between the surgical modalities and the simple drainage procedures, if hepatic resection could not be accomplished with bile duct resection. A few studies recently reported that the median survival time of patients who had a successful drainage with ERBD or PTBD was much longer than that of the patients who did not have a successful drainage[12,13]. Another recent study, mentioned above, suggested effective palliation by successful biliary drainage with subsequent TACE might prolong the survival in patients with obstructive jaundice caused by unresectable HCC[7].
In conclusion, we suggest that, for obstructive jaundice of inoperable HCC with biliary invasion, PTBD or ERBD should be considered as an initial management. After improvement of jaundice, TACE can be a successful modality for the resolution of bile drainage as a palliative treatment. And, a patient also can be expected to be sustained in resolved biliary occlusion without any other drainage device. Herein, we reported a case of a completely improved biliary invasion of HCC after TACE.
In conclusion, we suggest that, for obstructive jaundice of inoperable HCC with biliary invasion, PTBD or ERBD should be considered as an initial management. After improvement of jaundice, TACE can be a successful modality for the resolution of bile drainage as a palliative treatment. And, a patient also can be expected to be sustained in resolved biliary occlusion without any other drainage device. Herein, we reported a case of a completely improved biliary invasion of HCC after TACE.