INTRODUCTION
Anatomic variations in the biliary structure may go undetected until adulthood, and they can be the cause of unexplained jaundice or abdominal pain. In addition to such associated diseases as cholangitis, gallstones, cholangiocarcinoma, and pancreatitis, recognition of these variant anatomies is clinically important for planning surgery and for preventing inadvertent surgical injury [1]. For accurate treatment of biliary disease, a surgeon or endoscopist must consider variations in anatomy, as accidental ligation of an aberrant bile strictures or blood vessel can have a dramatic outcome, leading to sudden jaundice and bleeding. Congenital abnormalities and variations in the cystic duct are common, Talpur et al. [2] found that frequency of cystic duct variants is 4.33%. However, an accessory cystic duct draining into the right hepatic duct is rare. We report a case of an accessory cystic duct draining into the right hepatic duct with cholelithiasis, in which the abnormality was identified by endoscopic retrograde cholangiopancreatography (ERCP), magnetic resonance cholangiopancreatography (MRCP), and subsequently confirmed by laparoscopic cholecystectomy.
CASE
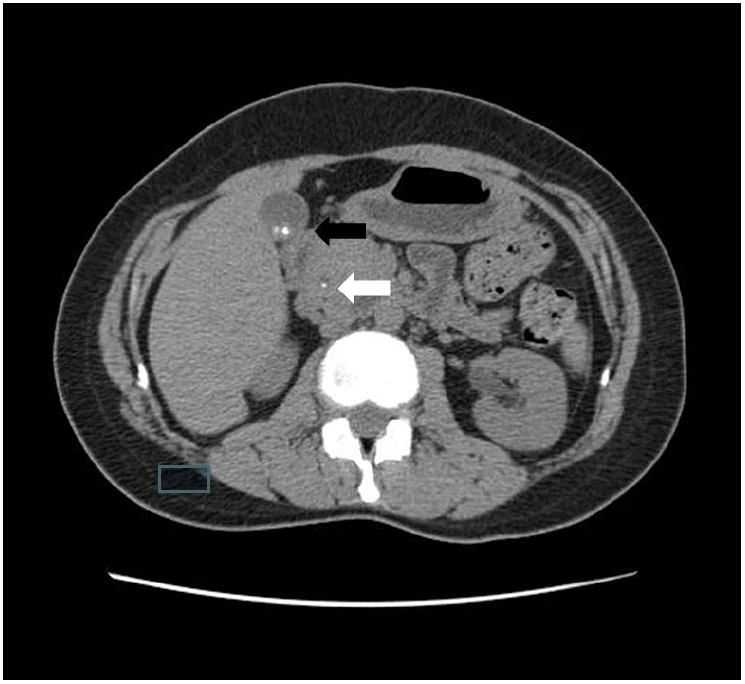
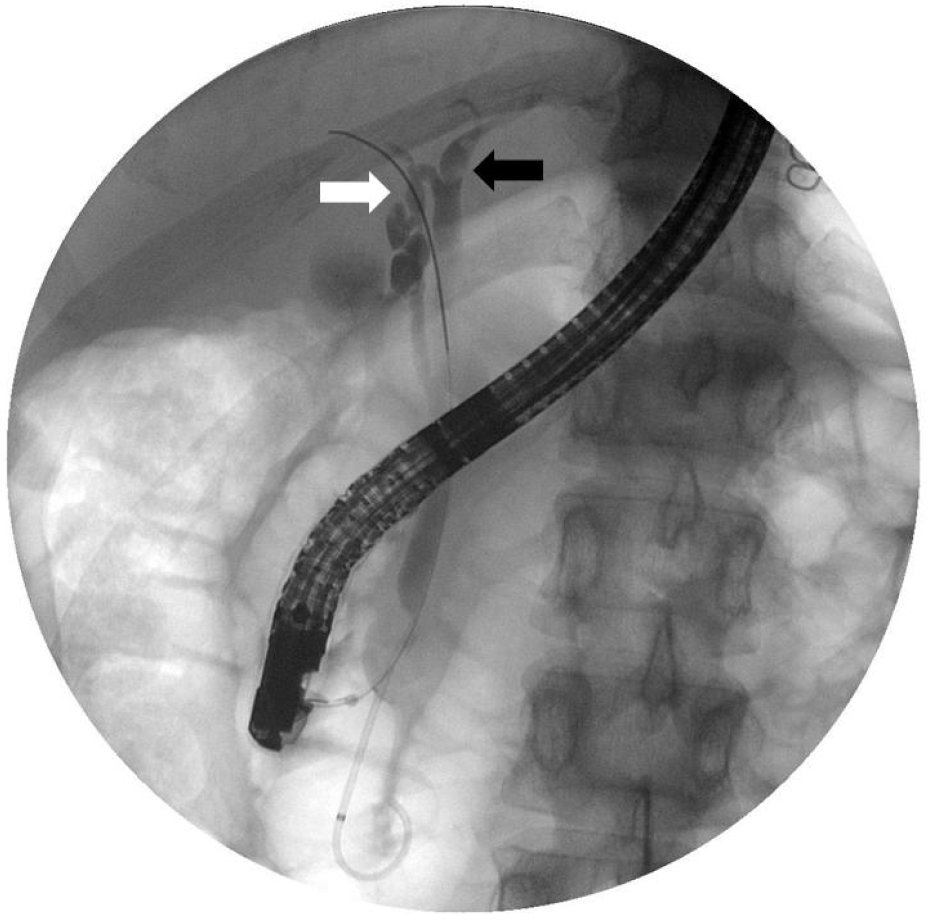
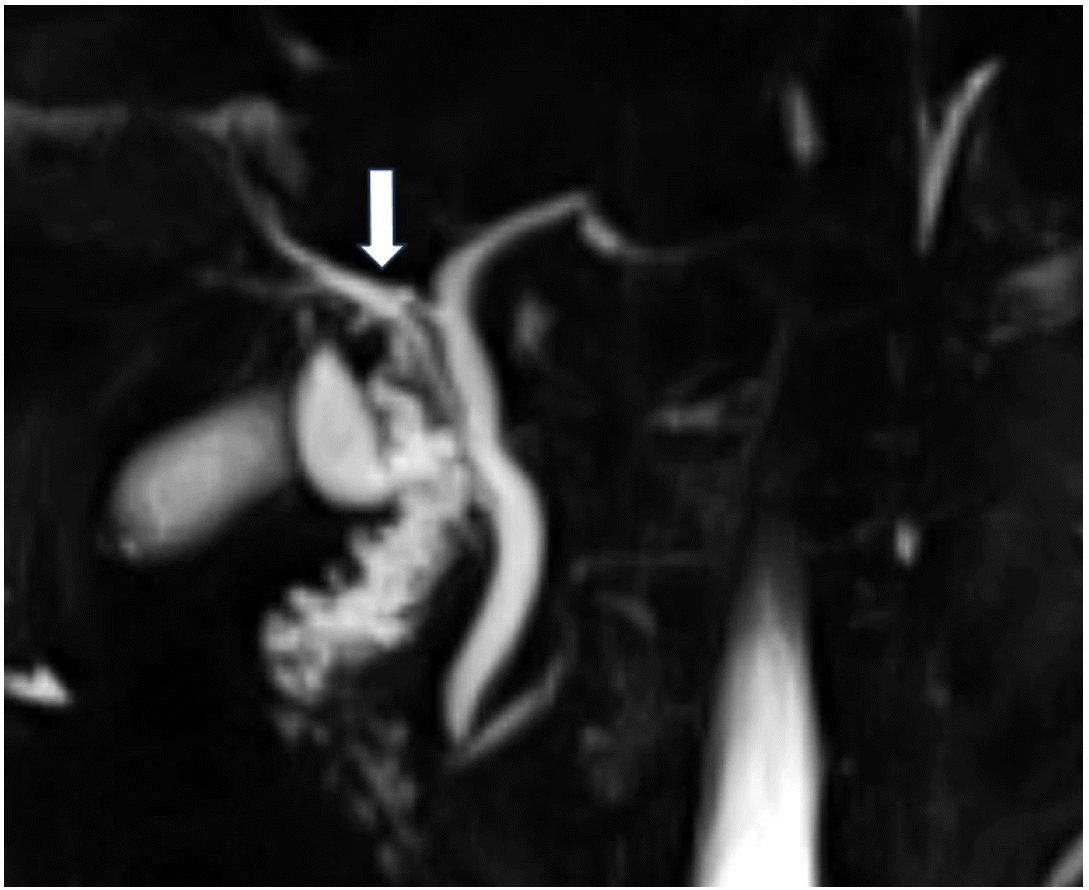
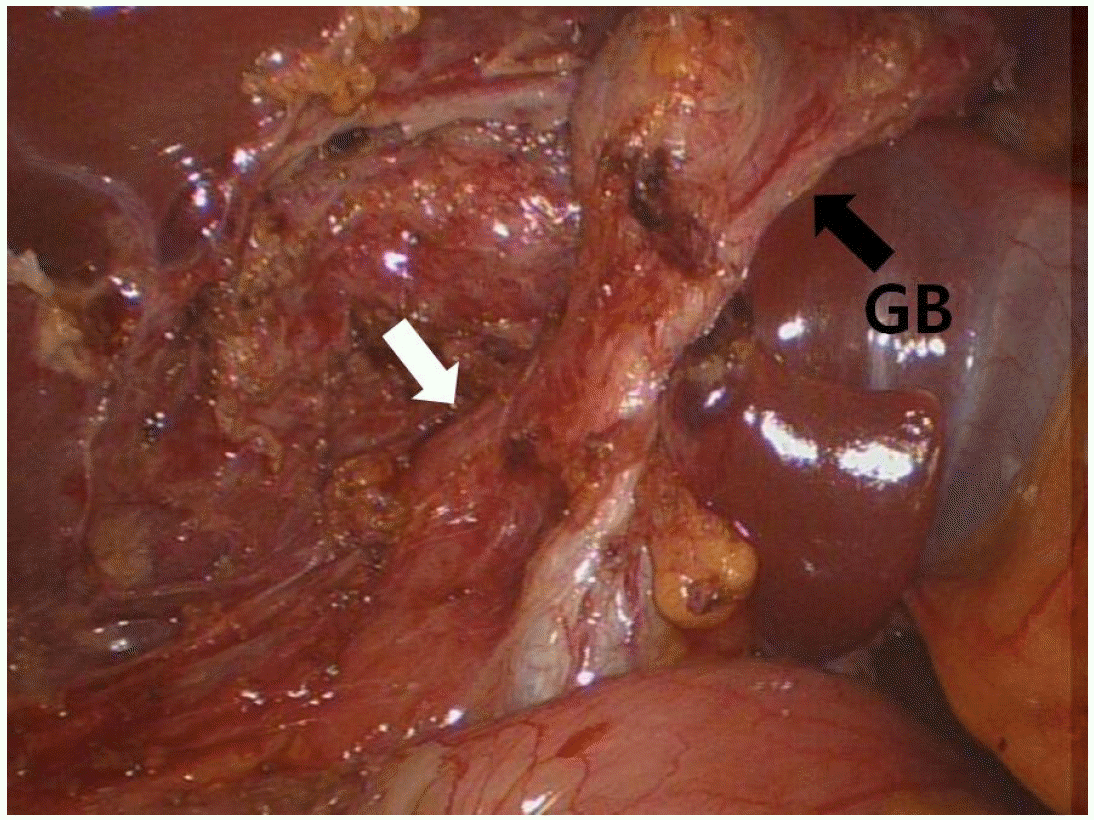
A 34-year-old woman was transferred to our hospital because of right upper quadrant pain for 2 months. She was diagnosed as chronic calculous cholecystitis by abdominal ultrasonography at another hospital. Past medical history was unremarkable. The patient was alert. The vital signs were stable. She had mild tenderness on the right upper quadrant but no jaundice on the sclera. In peripheral blood tests, white blood cells, hemoglobin, and platelets were within normal ranges. C-reactive protein and erythrocyte sedimentation rate had increased to 10 mg/dL and 20 mm/h, respectively. In biochemical tests, aspartate transaminase, alanine transaminase, total bilirubin, alkaline phosphatase, amylase, and lipase were normal at 25 IU/L (reference range 0-40 IU/L), 32 IU/dL (reference range 0-40 IU/L), 0.36 mg/dL (reference range 0.0-1.0 mg/dL), 95 IU/L (reference range 42-98 mg/dL), 64 IU/L (reference range 25-115 IU/L), 287 IU/L (reference range 73-393 IU/L), respectively. Gamma-glutamyl transpeptidase had increased to 80 IU/L (reference range 7-30 IU/L). An abdominal computed tomography (CT) scan demonstrated a tiny stone in the common bile duct and multiple gallbladder stones and cholecystitis (Fig. 1). ERCP was carried out on the next day, and a 3.6 mm sized filling defect was seen in the left hepatic duct. After endoscopic sphincterotomy, the stone in the left hepatic duct was removed with a balloon catheter. Cholangiogram obtained after stone removal showed an accessory cystic duct draining the right hepatic duct (Fig. 2). Subsequent MRCP showed no remaining stone and the same finding as that of endoscopic retrograde cholangiogram (Fig. 3). After a thorough discussion of the patient’s anatomic variant with the general surgeon, the patient underwent laparoscopic cholecystectomy. On careful dissection of the gallbladder from liver bed, a tubular structure was found running from liver bed to the body of the gallbladder. The tubular structure was clipped close to an accessory cystic duct and the gallbladder end was divided. A careful examination during the surgery confirmed the preoperative finding of an accessory cystic duct draining the right hepatic duct (Fig. 4). A pathological examination after the operation showed chronic cholecystitis. The patient was discharged without complications.
DISCUSSION
Anatomic variations in the biliary structure are a result of complex embryological development [3]. The biliary tract has more anomalies in 1 cm3 of space in the cystic duct region than any other part of the human body [4]. This anatomic variability usually creates difficulties for surgeons. Careful exploration of Calot’s triangle and an exact identification of the extra-hepatic biliary tree are important to avoid biliary complications during cholecystectomy. Failure to identify these differences may result in inadvertent ductal ligation, bile leak, or a stricture after the laparoscopic cholecystectomy. This result causes significant morbidity which has been reported to occur in 0.2–2% of cases after laparoscopic cholecystectomy [5]. To prevent these complications, surgeons must have a sound knowledge of the basic biliary tract anatomy as well as its surgical implications [6].
Retrospective study of intraoperative cholangiograms have shown up to 20% of patients have anatomical variations in the biliary tree [7]. Talpur et al. [2] found that frequency of cystic duct variants is 4.33%. The most common variation observed was a short cystic duct (2.67%), followed by a long cystic duct (1%), accessory cholecystohepatic duct (0.67%). This case was an accessory cystic duct draining into the right hepatic duct with chronic calculous cholecystitis. Kang et al. [8] reported a case of a cystic duct draining into the right hepatic duct along with acute pancreatitis.
It is difficult to diagnose these variants before cholecystectomy by routine investigations for gallbladder diseases. However, special investigations such as CT, percutaneous transhepatic cholangiography, ERCP, and MRCP are of value to delineate normal anatomy as well as cystic duct variants. In this case, we performed ERCP and MRCP.
However, these anomalies often turn out to be unexpected findings during laparoscopic surgery and are usually detected accidentally during an operation; thus, surgeons must identify all structures carefully. Failure to recognize certain anatomical variants may lead to bile duct damage resulting in serious morbidity and sometimes mortality [9]. The basis of major duct injury is the misidentification of the biliary anatomy during dissection of the cystic duct. In this case, there was a risk that the right hepatic duct may be mistaken for the accessory cystic duct and tied off and divided where it joins the left hepatic duct. Preoperative identification of the anatomic variant and a careful examination during the surgery prevented surgical complications.
In conclusion, congenital anomalies and anatomic variations of the cystic duct are not common but can be of clinical importance. Surgery carried out in ignorance of anomalies can result in major complications such as inadvertent ductal ligation, bile leaks, or strictures. Therefore, it is important to have a thorough knowledge to successfully detect and recognize such anatomic variations in order to decrease morbidity and mortality rates during hepatobiliary surgery.