INTRODUCTION
Colonoscopy is a commonly performed procedure to diagnose and treat colorectal diseases. Since it is generally considered a safe method [1], most complications include minor and transient gastrointestinal symptoms such as abdominal bloating and abdominal pain [2]. However, unusual serious complications requiring hospitalization or operation have been reported in some literature [3,4]. Acute cholecystitis is one of the serious complications after colonoscopy, and only 10 cases of it was previously reported without certain pathophysiology. Therefore, we present a case of acute cholecystitis caused by gallstones after screening colonoscopy.
CASE
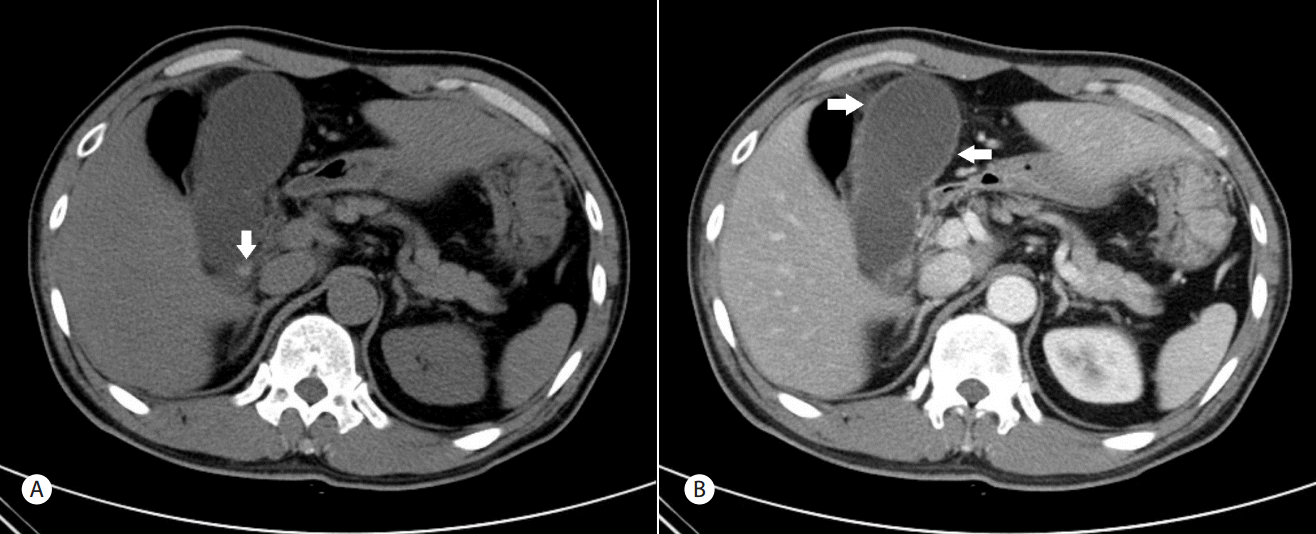
A 51-year-old male had undergone endoscopic retrograde cholangiopancreatography (ERCP) to remove common bile duct stones under the diagnosis of an acute cholecystitis 1 year earlier. He visited our hospital for regular health checkup including colonoscopy. He received 4 liters of polyethylene glycol solution for bowel preparation on the day before colonoscopy. He had no gastrointestinal symptoms. Colonoscopy were performed without difficulty and showed normal findings. After examination, he had no symptoms. About 40 hours after the procedures, he visited the emergency room with right upper quadrant abdominal pain and fever. Abdominal pain was gradually aggravated without other gastrointestinal symptoms. He showed the blood pressure of 148/85 mmHg, pulse rate of 78 beats per minute, respiration rate of 22 breaths per minute, and body temperature of 38.7°C. Upon abdominal physical examination, decreased bowel sound, tenderness and rebound tenderness of right upper quadrant abdomen and Murphy’s sign were observed. On laboratory examination, white blood cell count was 12,680/mm3, polymorphonuclear leukocytes was 83.2%, hemoglobin was 14.7 g/dL, platelet count was 151,000/mm3 and C-reactive protein level was 1.1 mg/dL. Blood chemistry analyses included total protein of 6.7 g/dL, albumin of 42 g/dL, aspartate aminotransferase of 25 IU/L, alanine transaminase of 17 IU/L, alkaline phosphatase of 37 IU/L, total bilirubin of 1.8 mg/dL, direct bilirubin of 0.3 g/dL, gamma glutamyl transpeptidase of 32 IU/L, lipase of 6 IU/L, and amylase of 60 IU/L. Chest and abdomen radiography were normal. Abdominal computed tomography (CT) showed faint gallstones in the neck of the gallbladder (Fig. 1A) and the enlarged gallbladder with mild diffuse wall thickening (Fig. 1B). After the diagnosis of acute cholecystitis, the patient was transferred to other hospital for personal reason. After 1 week, he had laparoscopic cholecystectomy and was discharged without any complications.
DISCUSSION
Complications of colonoscopy are increasing as the colonoscopy is widely used to screen and treat colorectal diseases. According to the study by Ko et al. [2], minor common complications after screening or surveillance colonoscopy included abdominal bloating and abdominal pain with incidence of 34%. Most minor complications were resolved in 2 days without any treatment. Nausea and electrolyte disturbance during bowel preparation, respiratory arrest and hypotension related to sedation were another minor complications [5]. On the other hand, rare but serious complications can also occur when invasive procedures are performed. Rabeneck et al. [3] reported that colon bleeding and perforation were most 2 common severe complications with incidence of 0.16% and 0.085%, respectively in 97,091 patients who underwent colonoscopy. Moreover, even colonoscopy-related death was reported in patient with high risk factors such as older age and history of polypectomy. Other possible serious complications contain post-polypectomy electrocoagulation syndrome, splenic rupture, acute appendicitis, diverticulitis and subcutaneous emphysema [3,4].
Acute cholecystitis as in our case is an extremely rare complication of colonoscopy. It was first described by Milman and Goldberg in 2001 [6]. Later, only 6 international cases were reported [7-9]. In Korea, 2 cases by Yun et al. [10] and Park et al. [11] were presented in 2013. In most cases abdominal pain and other gastrointestinal symptoms were developed within 72 hours after colonoscopy with additional procedure such as polypectomy or biopsies. Acute cholecystitis in those cases was diagnosed by abdominal sonogram or CT with the presence of gallstones, finally requiring cholecystectomy. In our case, although the patient underwent colonoscopy without any invasive procedures, right upper quadrant abdominal pain and fever were developed within 40 hours after colonoscopy. The patient showed the similar clinical course to that in previous studies and was diagnosed to have acute cholecystitis caused gallstones on abdominal CT (Table 1). We could not consider acute cholecystitis as the primary cause of the presenting symptoms. However, acute choelycystitis was ultimately suspected as the patient had aggravated abdominal pain with obvious Murphy’s sign and a prior history of removal of common bile duct stones.
The pathophysiology of acute cholecystitis after colonoscopy remains uncertain. It may be associated with serial procedures related to colonoscopy. Since it takes much time to form a new gallstone in the gallbladder, we suppose that the reported patients with cholecystitis after colonoscopy had previously existing gallstones or common bile duct stones. For our patient had a history of common bile duct stones, he had high risk for gallstones and possibly had remnant gallstones that had not been completely removed by ERCP. The mechanisms of development of acute cholecystitis suggested in previous reports are as follows. Firstly, dehydration arising from bowel preparation and fasting is associated with acute cholecystitis. Dehydration can cause decrease in bile flow, resulting in cholestasis. Cholestasis induces the enlargement of gallbladder and provides enough time for nucleation that is essential for formation of gallstone. Also, it alters the composition of bile by increasing the exposure to enteric bacteria. The altered composition of bile leads to the oversaturation of cholesterol and bilirubin which is fundamental for the formation of gallstones in gallbladder. The oversaturation of cholesterol and bilirubin increases the secretion of gallbladder mucin [12]. Besides, it decreases the contraction of gallbladder and causes the interruption in emitting small gallstones or crystals, ultimately facilitating the formation of gallstones [13,14]. Secondly, the 6-keto-prostaglandin F1-α is secreted more as intestinal epithelium is stimulated by solution for bowel preparation. It makes to increase the contractility of gallbladder. Accordingly, gallbladder directly displaces previously existing gallstones to the neck of gallbladder and arises the occurrence of choecystitis by obstruction of gallbladder [8,15]. Lastly, bacterial translocation via mechanically damaged colon mucosa during colonoscopy may cause cholecystitis by inflammation [6,7].
Transient abdominal bloating and abdominal pain are most common complications after colonoscopy. When severe abdominal pain and fever are present after colonoscopy, bleeding or perforation of colon should be first considered as serious complications. But, acute cholecystitis can also occur after colonoscopy, especially when patients had a history of gallstones. Therefore, we should carefully deal with the presented symptoms and consider the acute cholecystitis along with bleeding or perforation of colon as the complication after colonoscopy to prevent further fatal outcomes.