INTRODUCTION
The major papilla of duodenum typically enters the posteromedial side of the second portion of the duodenum [1]. The ectopic opening of common bile duct (CBD) is reported about up to 13%; which is located in the third, the fourth portion of the duodenum or duodenal bulb [1,2]. Nevertheless, the aberrant orifice of the CBD in the duodenal bulb is reportedly extremely rare (0.43%) and it is frequently associated with recurrent duodenal ulcer, bile duct stone, cholangitis, and gallbladder cancer [3]. However, there was no report of the malignant change of ectopic CBD orifice in the duodenal bulb yet. This is the first report of ectopic opening of the CBD into the duodenal bulb combined with precancerous change, high grade dysplasia. Herein, the pathogenesis and clinical features of aberrant opening of the CBD will be described in this paper.
CASE
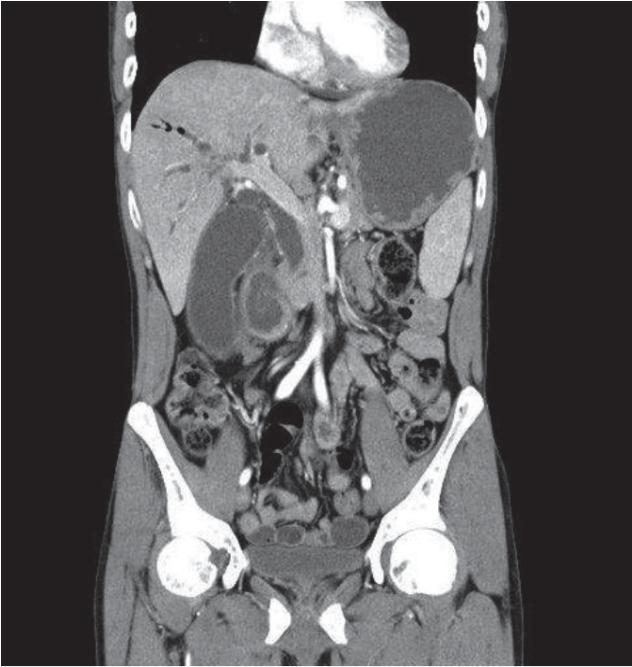
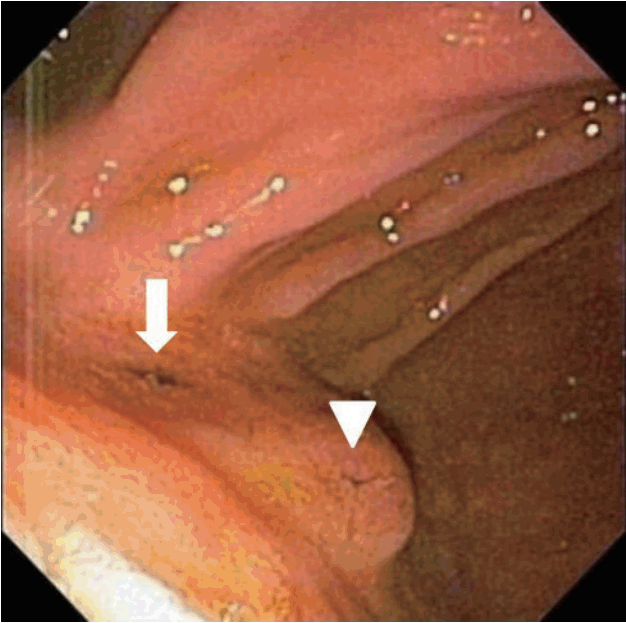
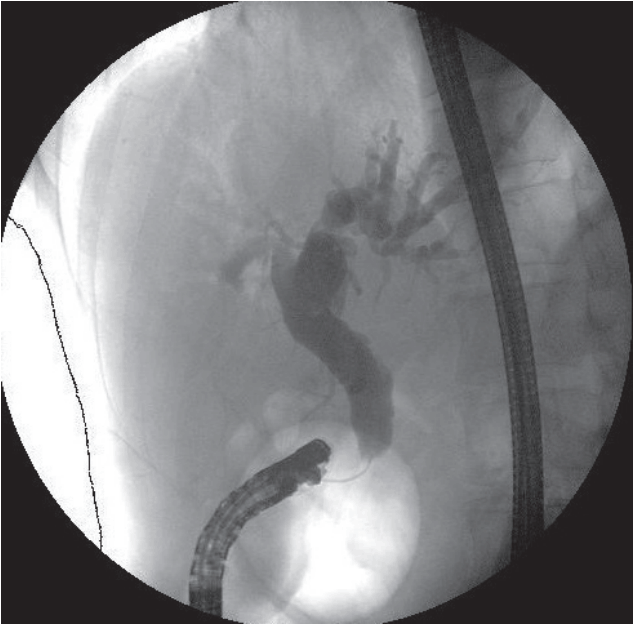
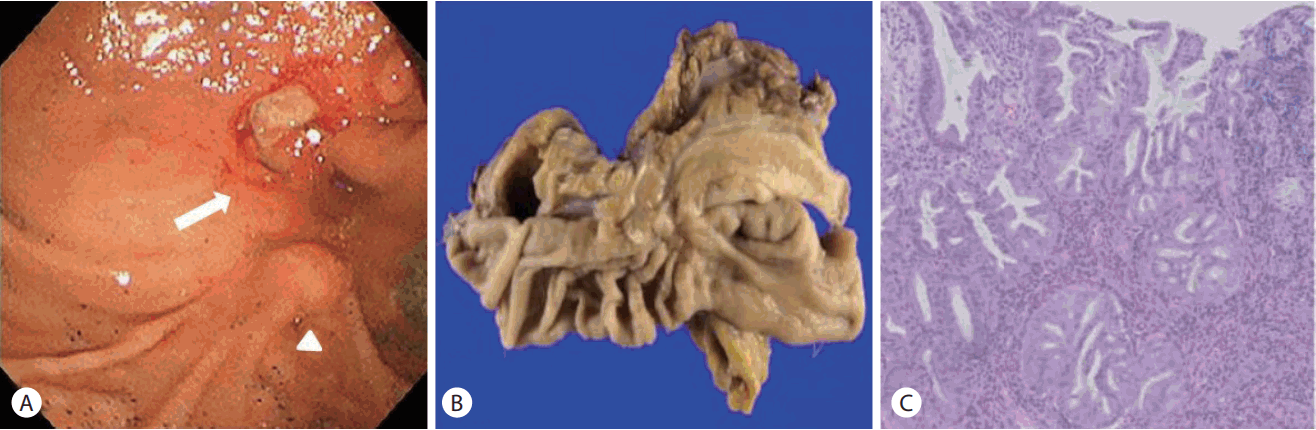
A 43-year-old male was referred to our emergency room because of epigastric pain for 3 days. He experienced a duodenal ulcer 10 years ago, without abdominal surgery. Physical examination showed mild right upper quadrant tenderness and blood chemistry revealed elevated serum total bilirubin 1.5 mg/dL, aspartate aminotransferase 15 IU/L, alanine aminotransferase 16 IU/L, alkaline phosphatase 607 IU/L, and gamma-glutamyl transpeptidase 283 IU/L. Computed tomography scan demonstrated intrahepatic pneumobilia and smooth tapering of distal CBD without obstructive lesion (Fig. 1). On upper endoscopy, a pseudodiverticulum with duodenal deformity at the bulb was visualized. There was a deformed ampulla of Vater (AOV) with slit-like opening at the upper mound of AOV (Fig. 2), suggesting fistular opening. It was considered as a stricture lesion of ectopic opening of CBD due to duodenal bulb deformity. Then, endoscopic retrograde cholangiopancreatography was performed. Repeated attempts to the cannulation via the ampullary orifice were failed due to the anatomical deformity. The cannulation catheter was successfully advanced through slit-like fistular orifice at upper mound of ampulla and then full cholangiogram was obtained (Fig. 3). With fistula opening using 6 mm-CRETM balloon dilator (CRETM PRO Wireguided; Boston Scientific, Cork, Ireland), the 7 Fr endobiliary stent was placed. He was discharged from hospital with improved symptoms. However, he was rehospitalized with aggravated jaundice two weeks later. The clogged plastic stent was changed into the nasobiliary catheter and biopsy was executed around the ampullary and fistular opening due to hyperemic mucosa with central ulceration (Fig. 4A). The pathology of specimen showed suspicious high grade dysplasia (Fig. 4B, C). and he underwent Whipple’s operation. The resected tissue was confirmed as high grade dysplasia of AOV without tumor invasion of the CBD or adjacent lymph nodes.
DISCUSSION
Anomalous drainage of the CBD into the duodenal bulb is not an incidental finding. It is related with clinicopathologic features, such as duodenal ulcer and recurrent cholangitis [4,5]. The etiology of atypical opening of the CBD has been described to unidentified errors in embryogenesis [1,6,7]. It occurs due to a disproportional elongation and early subdivision of the primitive hepatic furrow [6,7]. Clinical manifestations and complications of abnormal opening of the CBD into the bulb include biliary pain, recurrent or intractable duodenal ulcer, choledocholithiasis, obstructive jaundice, and liver abscess [5]. It is reported that dilated CBD with or without stone, pneumobilia and pancreatic duct dilation can be visualized in the cholangiogram [5]. In this case, the patient experienced several episodes of biliary colic and cholangiogram showed a diffusely dilated bile duct without stone and evident pneumobilia. Furthermore, histological examination of the AOV revealed the high grade dysplasia.
Two cases of uncommon openings of the bile duct associated with cancer have been reported; one is a periampullary carcinoma with ectopic ampulla opening into the 4th part of the duodenum [2] and another is gallbladder cancer with ectopic CBD opening into the duodenal bulb [3] (Table 1). To the best of our knowledge, our case is the first report of aberrant opening of the CBD in the duodenal bulb with precancerous change suggesting high grade dysplasia.
The pathogenesis of tumorous change at the ectopic orifice of the duodenal bulb has never elucidated, but plausible hypotheses are as follows [1]. First, the hook-shaped configuration of the distal CBD can interfere with the drainage of bile, which may be associated with bile stasis and recurrent cholangitis. Second, ectopic opening of the CBD might deform the typical configuration of the sphincter of Oddi and may form an abnormal slit-like orifice on the endoscopic examination [1]. Malfunction for the valve mechanism due to the absence of the sphincter of Oddi might lead to the recurrent reflux of intestinal bacterial and duodenal contents into the biliary system, which is related with recurrent cholangitis, liver abscess, and pneumobilia [5,8]. Repeated biliary stasis or recurrent reflux due to anatomical deformity may attribute to the development of precancerous lesion. A series of physical and chemical irritation by the duodenal contents including bacteria, which cause recurrent chronic inflammation, can result in dysplasia and even invasive carcinoma.
In patients with cholangitis with choledocholithiasis, endoscopic balloon dilatation may be the satisfactory treatment due to acute angulation of the distal CBD and intramural deformity of sphincter of Oddi [8,9]. However, in most patients, recurrent cholangitis and intractable duodenal ulcers can cause the stricture of the ectopic opening of the CBD, which frequently requires surgery [1,5]. Our patient was readmitted with recurrent cholangitis within 2 weeks due to malfunction of endoscopic retrograde biliary plastic stent. Abnormal findings of mucosa around the fistular opening and AOV were found and endoscopic biopsy was performed. Microscopic examination revealed high grade dysplasia and patient underwent Whipple surgery.
In conclusion, clinicians keep in mind that there is a possibility of dysplastic change in patient with the aberrant drainage of the CBD in the duodenum, especially in the presence of mucosal abnormality. Endoscopic biopsy should be recommended to rule out any malignant change in case of unusual opening of CBD if there is any color change or ulcerative lesion around mucosa.