INTRODUCTION
An arteriovenous malformation (AVM) is a composite tangle of abnormal arteries and veins linked by one or more direct communications called a fistula or shunt. Pancreatic AVM is defined as a tumorous formation or vascular anomaly built up via an aberrant bypass anastomosis of the arterial and venous systems in the pancreas [1]. Pancreatic AVM is an exceedingly rare condition and the true prevalence of the disease remains unknown [2]. Pancreatic AVM is mostly congenital and may be found without symptoms, but it may be discovered during a medical examination due to symptoms such as gastrointestinal bleeding or abdominal pain. Herein we report a case of acute pancreatitis due to pancreatic AVM with a retention cyst, in a 45-year-old-Korean male, which was successfully treated by surgical resection. We also review the literature relating to pancreatic AVM.
CASE
A 45-year-old Korean male was admitted to our hospital with symptom of epigastric pain for the past 5 days. He had been experiencing intermittent epigastric discomfort for the previous 2 months. He had no other medical history. He had no history of operation or trauma. No relevant family history, including diabetes and pancreatitis, was found.
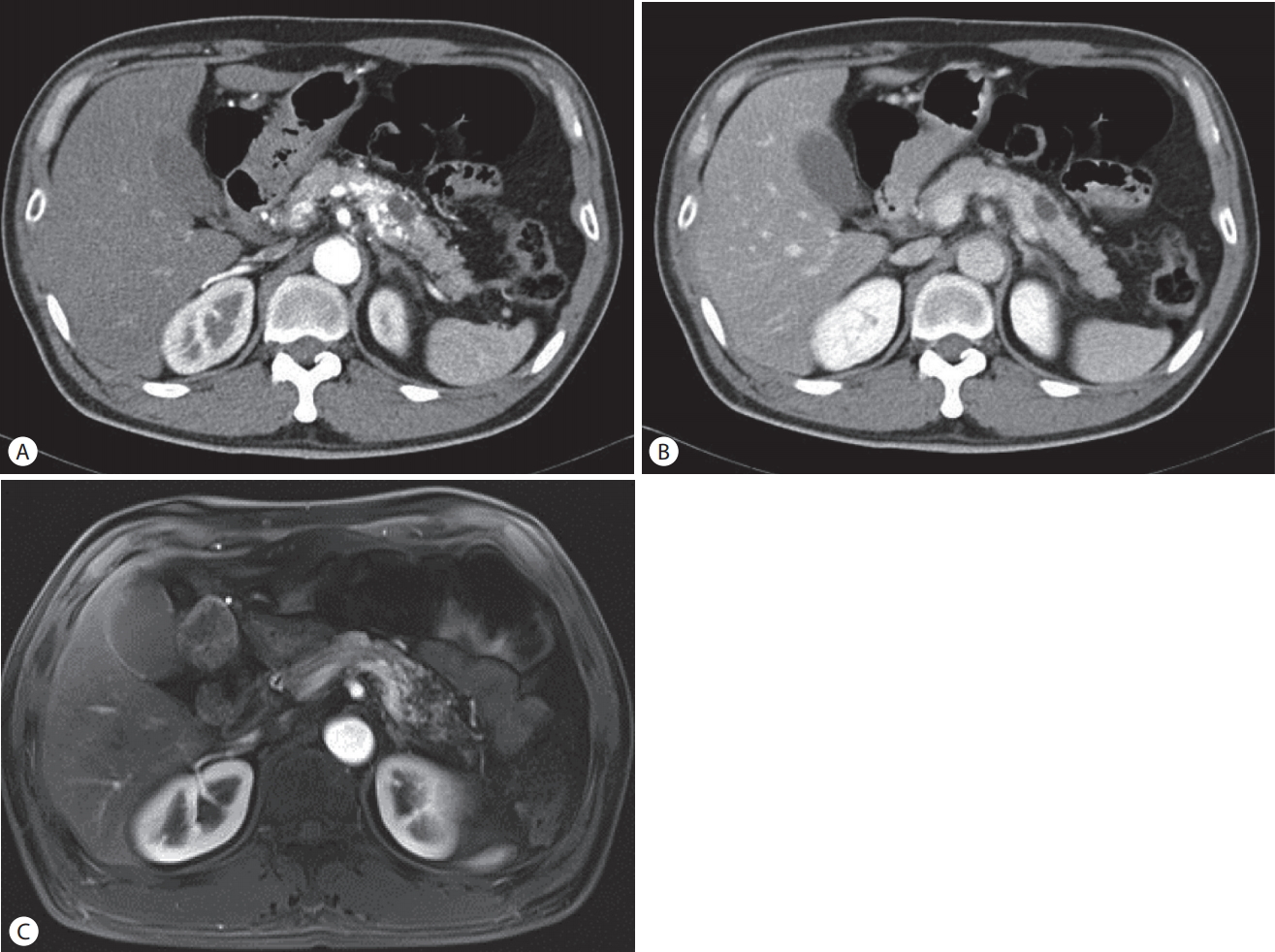
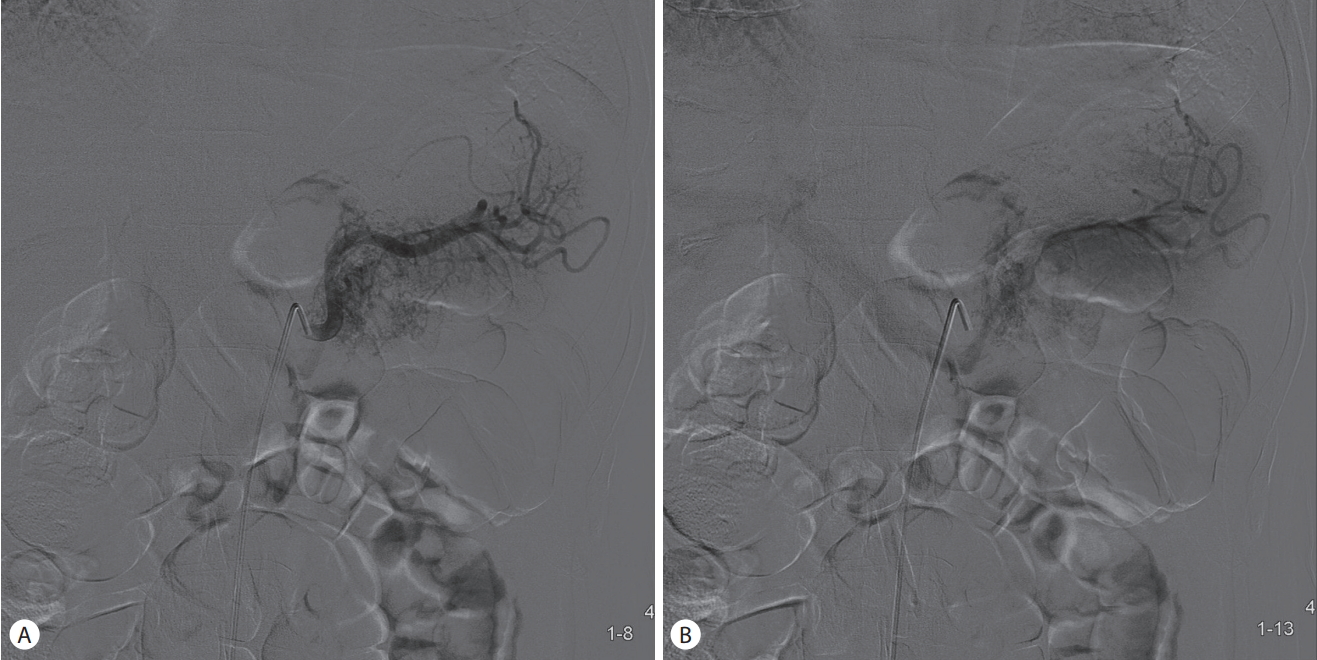
At the time of admission, the patient had an acute ill appearance, consciousness was clear, blood pressure was 130/80 mmHg, pulse rate was 72 beats/min, and body temperature was 36.5℃. The conjunctiva was not pale, and sclera had no jaundice. There were no specific details on chest auscultation, and heart sounds were regular. An abdominal examination revealed mild tenderness in the epigastric area and no other abnormal findings. He did not drink alcohol and had a 20 pack-years history of smoking. Laboratory studies revealed a white blood cell count of 14,410/mm3, a hemoglobin concentration of 18.3 g/dL, and a platelet count of 270,000/mm3. The result of liver tests are as follow: total bilirubin 0.99 mg/dL, alkaline phosphatase 75 IU/L, aspartate aminotransferase 16 IU/L, alanine aminotransferase 34 IU/L, total protein 7.4 g/dL, and albumin 4.5 g/dL. Amylase and lipase were elevated to 483 U/L and 492 U/L respectively. Triglyceride was 94 mg/dL. Serum electrolytes and coagulation were within normal range. The tumor marker test was carbohydrate antigen 19–9 35.98 U/mL (reference range, 0-37), and IgG4 was 703 mg/L (reference range, 30-2,010). On admission 2 days later, a contrast enhanced computed tomography (CT) scan of the abdomen to find the cause of the persistent pain showed suspicious pancreatic swelling in the body to the tail of the pancreas that corresponded to acute pancreatitis CT grade B. Irregular dilated vessels with a cystic lesion in the pancreatic body appeared on the arterial phase (Fig. 1A), but contrast enhancement of irregular vessels in the pancreatic body disappeared on the portal phase (Fig. 1B). A magnetic resonance imaging (MRI) scan of the abdomen on T1-weighted phase showed a strong enhancement of the congeries with a signal void in the pancreatic body with a unilocular cystic lesion (Fig. 1C). These findings suggested a focal acute pancreatitis and pancreatic AVM. Selective angiography was performed to confirm the diagnosis of pancreatic AVM. The angiography showed the proliferation of a vascular network in the pancreatic body and early visualization of the portal vein at the arterial phase (Fig. 2); these findings were compatible with pancreatic AVM. The cause of abdominal pain was diagnosed by acute pancreatitis caused by pancreatic AVM, and, for definitive treatment of symptomatic pancreatic AVM, distal pancreatectomy with splenectomy was performed. Intraoperatively, the distal portion of the pancreas was diffuse hard, and there was a solid lesion at the body of the pancreas, measuring 4×3 cm. On histologic gross sections, there was an ill-defined solid lesion with abundant vascularity and dilated spaces. The pancreatic duct was grossly unremarkable (Fig. 3A). A microscopic examination of the resected specimen showed hemorrhagic type acute pancreatitis, and a conglomeration of irregular dilated and tortuous arteries and veins in the pancreatic subcapsular tissue and parenchyma (Fig. 3B, C). A cystic lesion at the pancreatic body revealed a retention cyst with epithelial cell lining, which occurs when the pancreatic duct is dilated by obstruction (Fig. 3D). The patient was discharged 21 days after the operation. He tolerated post-surgery recovery well without any complaints of abdominal pain for 6 months of follow-up.
DISCUSSION
AVM in the digestive system is a rare disease, mainly found in the liver [3]. About 78% of AVM case of the digestive organs other than the liver were located in the cecum and right colon, followed by jejunum (10.5%), ileum (5.5%), duodenum (2.3%), stomach (1.4%) and rectum (0.9%), whereas only 0.9% were located in the pancreas [3]. Although the number of reported cases is increasing due to the widespread use of imaging techniques, the true prevalence of the disease is still unknown. In an AVM case series report, the median age at diagnosis was 50 years (range, 7 months to 75 years) with an Asian (78.3%) and male (88.4%) predominance [4]. The portion of the pancreas most frequently involved was the head (59.4%), followed by the body and tail (33.3%), and the entire pancreas (7.2%) [4].
The etiology of pancreatic AVM is classified as congenital and acquired. Congenital pancreatic AVMs are caused by the abnormal development of the arteriovenous plexus in the embryo, whereas acquired pancreatic AVMs are caused by pancreatitis, tumors, or trauma. A review showed that pancreatic AVM was congenital in more than 90% of cases. There was also an association with Rendu-Osler-Weber disease in 10-30% of cases [5]. In the present case, there was no family history of Rendu-Osler-Weber syndrome and no telangiectasia. Also, there was no history of pancreatitis, tumor, or trauma. Therefore, the present case appeared to be a congenital pancreatic AVM rather than AVM associated with Rendu-Osler-Weber disease.
Most patients with pancreatic AVM are asymptomatic. In previous reports, clinical symptoms included varying combinations of gastrointestinal bleeding (47%), abdominal pain (41%), jaundice (14%), among other symptoms [2]. The main symptom of pancreatic AVM is gastrointestinal bleeding associated with portal hypertension [6]. In a recent study analyzing 89 cases reported in the literature [7], it was noted that the most common symptom of pancreatic AVM was gastrointestinal bleeding (47%), followed by epigastric pain (46%). It was also seen that, in the pancreatic head AVM group, bleeding was the most common complication, while in the pancreatic body-tail AVM group, pancreatitis was more common [7], as in the present case.
The case of pancreatic AVM with pancreatitis is a reported minority. The pathophysiology of pancreatitis with pancreatic AVM has not yet been clarified. The mechanisms of pancreatitis arising from pancreatic AVM may be classified into three types: i) by bleeding from pancreatic AVM extending into the pancreatic duct [8], ii) by ischemic injury due to the pancreatic AVM “stealing” flow from normal surrounding parenchyma like brain AVM [6], iii) by pancreatic duct compression from pancreatic AVM [9]. In the present case, like in most of the other previously reported case, pancreatic AVM and pancreatitis were detected simultaneously with no history of trauma or tumor in the patient, suggesting that the pancreatic AVM was congenital. In addition, acute pancreatitis was thought to be caused by the third mechanism, because the retention cyst occurring when the pancreatic duct was dilated by obstruction was observed.
Diagnosis is usually confirmed by imaging, because the symptoms are not specific, and the incidence of pancreatic AVM is low [10]. Radiographic examinations used for pancreatic AVM diagnosis include contrast enhanced CT, abdominal ultrasound, angiography, and MRI. The features of pancreatic AVM identified by multiphase contrast-enhanced CT include congeries of strong nodular stains and early contrast filling of the portal vein during the arterial phase [2]. A contrast-enhanced MR study may show similar findings as a dynamic CT study. Further, T1- and T2-weighted images can demonstrate arteriovenous malformation as multiple signal voids [2]. A definitive diagnosis is established using angiographic evaluation. The angiographic findings of pancreatic AVM are characterized by dilated and tortuous feeding arteries, a racemose intra-pancreatic vascular network followed by a transient dense pancreatic stain, early venous filling (into the portal vein), and early disappearance of the pancreatic stain [11]. In this case, the findings on CT and angiography were compatible with pancreatic AVM as stated above. Therefore, we could conclude that this case was a congenital AVM of the pancreas, leading to the development of acute pancreatitis.
Owing to the rarity of this disease, there are no standard management protocols and a wide range of strategies including both surgical and non-invasive therapies (e.g., arterial embolization, irradiation, transjugular intrahepatic portosystemic shunt) have been employed in the treatment of symptomatic patients [5]. Generally, pancreatic AVMs contain multiple feeding arteries, making it difficult to achieve complete embolization or ligation [12]. Awareness of complication risks caused by embolization, such as bowel ischemia resulting from distal organ embolization, is important. Incomplete treatment of pancreatic AVM such as arterial embolization, can result in growing new collateral vessels and cause the progression of portal hypertension, leading to recurrent gastrointestinal bleeding and/or rupture of the esophageal varices [4]. Furthermore, it has been reported to be impossible to reduce portal hypertension, once established, even if the pancreatic AVM is surgically removed [5]. Therefore, the definitive treatment for symptomatic AVM of the pancreas is surgical resection of the affected pancreatic lesion at an early stage, because it eliminates the cause of pain and prevents the development of portal hypertension [4,5]. When a patient is at a high surgical risk, arterial embolization, irradiation, and transjugular intrahepatic portosystemic shunt are alternative options [4].
In summary, we experienced a rare case of a 45-year-old Korean male who had acute pancreatitis associated with pancreatic AVM, which was diagnosed by dynamic contrast imaging, especially angiography, and successfully treated by surgical resection. Pancreatic AVM is extremely rare; even rarer is its association with pancreatitis. However, pancreatic AVM should be considered as another potential cause of acute pancreatitis.